Thrombophilia
Understanding Thrombophilia
If you or a family member has experienced a dangerous blood clot, you may have an underlying condition known as thrombophilia. Thrombophilia increases the risk for dangerous clots in your arms, legs and lungs. Some people are born with thrombophilia (inherited thrombophilia), while other people develop thrombophilia later in life (acquired thrombophilia). In either case, the condition has many forms and may affect people in different ways.
Many individuals with thrombophilia may never have a clotting problem, while others may experience a life-threatening clot or even a series of them. The good news is that close to 90 percent of all people with thrombophilia never develop a blood clot.1 In fact, they may live their whole lives without even knowing they have this risk. Unfortunately, however, certain types of thrombophilia do carry much higher risks.2
This resource provides a thorough overview of thrombophilia and its many forms, discusses the risks and potential complications, summarizes the current perspectives about testing and diagnosis, and provides an overview of potential treatment options and lifestyle adjustments that you and your physician may consider necessary.
With this information, we also share the experiences and insights of people who have been diagnosed with thrombophilia, as well as medical and scientific professionals experienced in diagnosing and managing clotting disorders.

Clotting
The Importance of Clotting
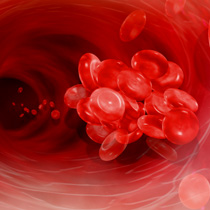
Blood clotting is essential to survival. Without it, the body is unable to stop bleeding after injury, illness or surgery. Even a minor injury or wound could progress to a medical emergency if clotting is inadequate.Normal clotting occurs in a series of reactions that work together to contain blood leaking out of damaged veins and arteries. When an injury happens, the body releases chemicals that constrict ruptured blood vessels, limiting blood flow to the area and reducing the size of the tears in vessel walls. The blood that has already spilled into the surrounding tissue forms a pool – called a hematoma – that presses against the vessels to further contain bleeding. These mechanical effects supplement the process by which the body manufactures its own clot to seal and begins healing the injury site.
When an injury happens, the body mobilizes cells called platelets that rush to the injury site and perform their valuable clotting function. Platelets stick to the vessel walls and to each other, forming a plug that seals the bleeding site and helps start the healing process. This complex process involves dozens of factors, proteins and enzymes. Defects in the production or performance of any of these substances can lead to clotting problems that will be discussed in subsequent sections.
Common Problem
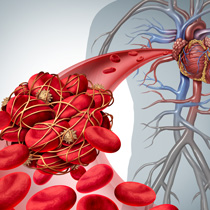
Venous Thromboembolism (VTE): A Common Clotting Problem
Although blood clotting is instrumental to survival and overall health, abnormal clotting can lead to serious medical problems. One of the most common clotting disorders is the formation of a harmful clot that blocks blood flow within a blood vessel, most usually a large vein in an arm or leg, known as a deep-vein thrombosis (DVT). If a DVT breaks away from its primary site and moves to the lung, it is known as a pulmonary embolism (PE). These are life-threatening and result in up to 100,000 deaths annually in the United States.If you experience the signs and symptoms of a blood clot in your leg or arm, you should contact your doctor as soon as possible. If you have the signs of a PE, which can be life-threatening, you should seek immediate medical attention.

Blood Clot Signs and Symptoms
DVT and PE have different symptoms that may sometimes be confused with other less serious health problems. For example, the cramping often characteristic of a DVT in the thigh can be interpreted as a “Charlie horse.” The breathlessness from a PE can be mistaken for allergies or anxiety. Only your doctor can accurately assess the presence or absence of a blood clot, so seek medical attention promptly if you experience any of the following signs or symptoms:
- Swelling of your legs or arms
- Pain or tenderness not caused by an injury
- Skin that is warm to the touch
- Redness or discoloration of the skin
- Difficulty breathing
- Chest or back pain that worsens with a deep breath
- Coughing or coughing up blood
- Faster than normal or irregular heartbeat
- Dizziness or feeling faint
Blood Clot Risks
Despite advances in blood clot treatment and prevention, clots remain a significant public health concern and continue to occur at relatively high rates – comparable to the incidence of stroke,3 the No. 4 killer in the United States.4 According to the U.S. Centers for Disease Control and Prevention, up to 900,000 people in the U.S. experience a blood clot each year, and about 100,000 die, many within a month of diagnosis. Of survivors, 30 percent will experience a recurrence within 10 years.5Blood clots are a leading cause of preventable death, particularly in people who are hospitalized. Approximately 50 percent of all blood clots occur during or within 3 months of hospitalization or surgery. Yet many hospitalized patients do not receive proper prevention.6
Although blood clots can occur at any age, risks increase with age. Researchers know that men are at a higher risk for blood clots than women.7 However, pregnancy, childbirth and use of estrogen-based contraceptives increase the chances for blood clots in women of childbearing age compared to non-pregnant women or women who don’t use these types of contraceptives. In fact, pregnant women have 5 times the risk for VTE than non-pregnant women of childbearing age. That risk actually increases about 20-fold in the weeks immediately following childbirth, and is at its highest – a risk of 100-fold – in the first week after the baby is born.8
For a comprehensive list of VTE risk factors, click this link to the National Blood Clot Alliance website: https://www.stoptheclot.org/know-your-risk.
Sometimes people experience blood clots for no apparent reason. These individuals may have a hidden risk for blood clots called thrombophilia. A thrombophilia can also be a risk factor that is present in addition to the ones listed above.
This web resource was produced specifically to help people with thrombophilia understand their condition, assess their risks in partnership with their doctor and take action to protect themselves when necessary. The subsequent sections will provide an overview of thrombophilia, the condition’s various sub-types, and the options for proper diagnosis and preventive treatment.
Hidden Risk
Thrombophilia: A Hidden Risk for Blood Clots
Some individuals have an underlying vulnerability for blood clots known as thrombophilia. Medical professionals often suspect the presence of thrombophilia whenever blood clots occur for unexplained reasons or when no other risk factors are present. About 30 percent of all people who experience a blood clot have no known risk factors, and in about half of these cases of unprovoked clots, thrombophilia is identified.9 Doctors will also consider thrombophilia when a blood clot occurs in a young person or in an unusual area of the body, such as the brain or abdomen. A history of multiple pregnancy losses may also be indicative of a concealed thrombophilia, specifically an autoimmune condition termed Antiphospholipid Syndrome (APS).The term “thrombophilia” encompasses a group of conditions characterized by abnormalities in various proteins that contribute to the clotting process. These abnormalities may involve any of the following features:
- Production of too much clotting protein
- Production of too few proteins that stop clotting
- Defective proteins that can resist breaking down after the need for clotting has passed
- Generation of amino acids that damage blood vessel walls and trigger clotting

(For a more comprehensive discussion of DNA basics, including how mutations occur, click this link: https://www.stoptheclot.org/news/the-genetics-of-thrombophilia/)Inherited thrombophilia is most often seen in people of Northern European descent and in certain Middle Eastern populations. It is rare among Asians, Africans and Native Americans.10Although thrombophilia increases one’s risk for a blood clot, it by no means guarantees one. The lifetime risk of developing DVT is 10 percent or less for certain thrombophilias,11 but the degree of risk fluctuates based on a number of considerations, including:
- Thrombophilia type. The various forms of thrombophilia are defined by the specific clotting protein the body produces irregularly. Some thrombophilias are more inherently dangerous than others. For example, thrombophilia characterized by hereditary antithrombin (HAT) deficiency is highly correlated with multiple blood clot episodes. More common forms, such as factor V Leiden and prothrombin G20210A (discussed in detail in the next section) increase the chance of a primary blood clot several-fold, but in the absence of other risk factors, the overall incidence of VTE with these two types of thrombophilias remains low.
- Degree of abnormality, as measured by the number of defective genes inherited. You receive two copies of every gene, one from each parent.
- Heterozygous. If only one thrombophilia-related gene in the pair is defective, your thrombophilia is considered heterozygous, and your body will produce 50 percent abnormal protein.
- Homozygous. If both parents have the same mutation, you could inherit two defective genes. In this case, your thrombophilia is homozygous. As a result, your body will produce 100 percent abnormal protein.
- Compound heterozygous. If you inherited a bad copy of one thrombophilia gene from one parent and a different thrombophilia gene from your other parent, your thrombophilia is considered compound heterozygous. For example, having one bad copy of factor V Leiden and one bad copy of Prothrombin Gene mutation is considered compound heterozygous.
Heterozygous conditions may increase your blood clot risk several-fold. On the other hand, homozygous conditions may multiply your risk by as much as 25 to 50 times the norm.12
- Other VTE risk factors. When thrombophilias are present in combination with other known blood clot risks, particularly hospitalization, surgery, pregnancy, cancer, or use of estrogen-based medications, the odds of a blood clot are greatly magnified. For example, some thrombophilias raise VTE risks 5 to 7 times the normal rate seen in the general population.13 Likewise, use of estrogen-containing oral contraceptives increase blood clot risks four-fold. But women with thrombophilia who use these OCs may face a 2- to 20-fold higher risk of an initial blood clot than women who do not use OCs.1415 The risk of a blood clot can also be magnified by obesity or smoking.
Types
Currently Recognized Thrombophilias
Most thrombophilias are characterized by the lack of adequate amounts of properly functioning clotting proteins. These conditions are either inherited genetically from one or both parents, or acquired as the result of injury, illness or surgery.
Hereditary Thrombophilia
Often, thrombophilias are inherited from one or both parents. Certain genetic mutations correspond with specific thrombophilias. Some mutations, such as those underlying factor V Leiden and Prothrombin G20210A, are relatively common, affecting 1-5 percent of the general population. Others, such as those responsible for protein C and protein S deficiencies, are less common, affecting fewer than one percent of people. Some thrombophilias are seen mostly in specific population subgroups or are very rare, posing little risk to the general public.

The following is a brief summary of some of the better-known inherited thrombophilias:
- Factor V Leiden: Named after the city in the Netherlands in which the genetic mutation was first identified, Factor V Leiden is the most common thrombophilia, occurring heterozygous (i.e., one defective gene copy) in approximately 5 percent of the Caucasian population and homozygous (i.e., two defective gene copies) in less than 1 percent. Hispanic Americans and African Americans are affected less often (2% and 1% prevalence, respectively) As with most thrombophilias, it is rare in people of Asian, African or Native American descent.16Factor V Leiden causes a genetic mutation that generates an abnormal version of factor V. As an instrumental clotting protein, factor V helps generate fibrin, the fibrous material that creates a “net’ to hold a blood clot together. Once a functional blood clot has been completed, factor V is inactivated by another substance called activated protein C – also known as APC. The altered version of factor V is resistant to APC, so its activity continues beyond its period of usefulness. As a result, factor V Leiden can cause an exaggerated clotting response.
The heterozygous form of factor V Leiden increases the risk for a first DVT 5- to 7-fold (i.e., an additional 5 to 7 people per thousand each year as compared to a 1 in 1,000 risk for the general population). However, the homozygous form increases blood clot risk by as much as 50-fold.17
- Hereditary Antithrombin Deficiency (HAD): Discovered in the 1950s, antithrombin is a protein that is necessary to prevent blood clots. People whose bodies don’t produce enough antithrombin are much more likely to develop a blood clot.HAD is less common than factor V Leiden. It occurs in about 0.02 % of the general population, or 1 out of 5000 people in the U.S. There are approximately 66,200 people in the USA that have this mutation. However, this is an estimate. It is the highest risk thrombophilia in terms of causing clots in the affected population. About 50% of people with antithrombin deficiency will have at least one clot by age 50. About six in 10 people with HAD will have recurrent blood clots. The presence of HAD can be established with a blood test. You may be at risk for HAD if you have already had a clot, particularly if the clot did not have an obvious cause or if it was unusual in some way, or if you have a family member with a history of clots. Similar to protein C and protein S deficiency, HAD can be caused by genetic mutations that result in either inadequate production of antithrombin or production of dysfunctional antithrombin. Both types result in deficient antithrombin activity and an increased risk of blood clot formation.
Blood clots with antithrombin deficiency occur at an average age of 30 and can appear in unusual locations, such as the veins of the brain or gastrointestinal tract, or in multiple veins simultaneously. Approximately 50 percent of people with HAD will experience a blood clot in their lifetime19 and 40 percent will experience a pulmonary embolism specifically. HAD increases the risk of blood clots by 20 percent compared to the general population.20
People with HAD are often treated by getting extra antithrombin to compensate for the antithrombin that is missing from the body. Treatment is more common in certain high-risk situations such as surgery, pregnancy and childbirth, or when the person already has a blood clot.
-
Factor V Leiden: Named after the city in the Netherlands in which the genetic mutation was first identified, Factor V Leiden is the most common thrombophilia, occurring heterozygous (i.e., one defective gene copy) in approximately 5 percent of the Caucasian population and homozygous (i.e., two defective gene copies) in less than 1 percent. Hispanic Americans and African Americans are affected less often (2% and 1% prevalence, respectively) As with most thrombophilias, it is rare in people of Asian, African or Native American descent.16
Factor V Leiden causes a genetic mutation that generates an abnormal version of factor V. As an instrumental clotting protein, factor V helps generate fibrin, the fibrous material that creates a “net’ to hold a blood clot together. Once a functional blood clot has been completed, factor V is inactivated by another substance called activated protein C – also known as APC. The altered version of factor V is resistant to APC, so its activity continues beyond its period of usefulness. As a result, factor V Leiden can cause an exaggerated clotting response.
The heterozygous form of factor V Leiden increases the risk for a first DVT 5- to 7-fold (i.e., an additional 5 to 7 people per thousand each year as compared to a 1 in 1,000 risk for the general population). However, the homozygous form increases blood clot risk by as much as 50-fold.17
-
Hereditary Antithrombin Deficiency (HAD): Discovered in the 1950s, antithrombin is a protein that is necessary to prevent blood clots. People whose bodies don’t produce enough antithrombin are much more likely to develop a blood clot.
HAD is less common than Factor V Leiden, affecting between 1 in 500 to 5000 people.18 This range suggests that approximately 63,000 to 630,000 people in the United States could be affected. However, it is the highest risk thrombophilia in terms of causing clots in the affected population. More than eight out of ten patients with HAD will have at least one clot by age 50. About six in ten people with HAD will have recurrent blood clots. The presence of HAD can be established with a blood test. You may be at risk for HAD if you have already had a clot, particularly if the clot did not have an obvious cause or if it was unusual in some way, or if you have a family member with a history of clots. Similar to protein C and protein S deficiency, HAD can be caused by genetic mutations that result in either inadequate production of antithrombin or production of dysfunctional antithrombin. Both types result in deficient antithrombin activity and an increased risk of blood clot formation.
Blood clots with antithrombin deficiency occur at an average age of 30 and can appear in unusual locations, such as the veins of the brain or gastrointestinal tract, or in multiple veins simultaneously. Approximately 50 percent of people with HAD will experience a blood clot in their lifetime19 and 40 percent will experience a pulmonary embolism specifically. HAD increases the risk of blood clots by 20 percent compared to the general population.20
People with HAD are often treated by getting extra antithrombin to compensate for the antithrombin that is missing from the body. Treatment is more common in certain high-risk situations such as surgery, pregnancy and childbirth, or when the person already has a blood clot.
- Prothrombin G20210A: Discovered in 1996, Prothrombin G20210A is the second-most common thrombophilia, occurring in heterozygous form in 2 percent of the Caucasian population.21 Less than 1 in 10,000 have the homozygous form. As with factor V Leiden, Prothrombin G20210A is rare in people of non-European or Middle-Eastern descent. Its name includes the code designating the exact location of the mutation within the DNA molecule. Prothrombin G20210A features a mutation in the gene responsible for production of prothrombin – also known as factor II – a protein like factor V that plays a critical role in the generation of fibrin – again, the material that constitutes the structural meshwork in a blood clot. Individuals with the heterozygous disorder have too much circulating factor II, increasing the odds of VTE by 2 or 3 times the normal blood clot risk.22 Scientists have yet to quantify the risk for the homozygous form.
- Protein C deficiency: First described in the medical literature nearly 40 years ago, protein C deficiency is a relatively uncommon thrombophilia, occurring in less than half of 1 percent of the population or 1 in 200-300 people in its heterozygous form.23 However, when it does appear, homozygous protein C deficiency is considered a life-threatening illness.24 Unlike factor V- and prothrombin-based thrombophilias, protein C deficiency is correlated with an elevated risk of recurrent blood clots. As a result, it may require more concern in those who have already experienced an initial VTE event. Protein C is instrumental to shutting down the clotting process once repair of a damaged blood vessel is completed. Individuals with a protein C-related mutation produce either too little of the protein or a version that is inactive.
- Protein S deficiency: This protein’s name stems from the city in which the protein was discovered, Seattle. Protein S is known as a co-factor in coagulation. By itself, it cannot produce the chemical reactions necessary to regulate blood clotting. Instead, it enhances the activity of other proteins and enzymes that have direct impact on the process. Individuals with this condition lack enough functional protein S in their circulation. As with other thrombophilias, mutations can occur to one or both gene copies. The milder heterozygous deficiency affects less than a quarter of 1 percent of the population (1 in 500).25 The life-threatening homozygous form is extremely rare, but is usually the culprit in purpura fulminans, an often lethal and systemic clotting disorder in infants.
- Homocystinuria: An inherited disorder, homocystinuria is characterized by the body’s inability to metabolize certain amino acids – particularly homocysteine – that are the building blocks of proteins. This defect leads to chronic elevations of homocysteine that can injure the interior walls of blood vessels and trigger blood clots. Blood clots in the arterial circulation, such as heart attacks or strokes, are more common that blood clots in the veins in people who have very high homocysteine levels in their blood. A mutation in the methylenetetrahydrofolate reductase (MTHFR) gene can elevate homocysteine levels and was once thought to increase the risk of venous thrombosis. However larger studies do not support an association between the most common MTHFR gene variants and the risk of thrombosis. Medical experts no longer suggest testing for MTHFR gene mutation when testing for inherited thrombophilia.
Acquired Thrombophilia
In acquired thrombophilias, an organ responsible for producing or eliminating these proteins, such as the liver or kidney, may have been damaged or altered by a major health event. As a result, the organ either doesn’t produce enough functioning protein or clears it too quickly from the blood before it can complete its work. In other instances, an illness, injury or toxic exposure can activate the over-production of chemicals that cause an imbalance in the clotting process.A prime example of an acquired thrombophilia is antiphospholipid syndrome (APS), a condition that poses particular risks for pregnant women because APS-related blood clots occur most frequently in advance of – or in the weeks following – childbirth. It can lead to miscarriage. Unlike most thrombophilias, APS is associated with a higher incidence of recurrent venous blood clots as well as arterial blood clots.27
APS is considered an autoimmune disease in which the body attacks its own cells, mistaking them for foreign invaders. The ensuing onslaught injures blood vessel walls, leading to exaggerated clotting responses.
People with other underlying autoimmune diseases, such as lupus, or a history of particular infections are at higher risk of developing APS.
Other acquired situations that can increase the risk of thrombosis include having active cancer, receiving anti-cancer treatments, recent surgery, immobility, or long travel. Hormone medications that include estrogen also increase the risk of developing a blood clot, as does being pregnant or recently postpartum.
Testing & Diagnosis
Thrombophilia Testing and Diagnosis
The value of testing for thrombophilia is a matter of continued debate within the medical community and among families. To date, no validated testing guidelines have yet been published. Data showing the clinical usefulness of thrombophilia testing are limited, as are the benefits of preventive blood clot treatment based on thrombophilia diagnosis alone.28Individuals with a confirmed thrombophilia may need to take special precautions when facing surgery, planning a pregnancy, anticipating an extended period of immobilization or choosing a contraceptive method or menopause treatment. These and other VTE risk factors can be especially concerning in combination with a known thrombophilia. Sometimes, your doctor may prescribe short-term, preventive therapy until these risks are resolved.
Testing may be helpful in people for whom the suspicion of thrombophilia is realistically high, including those who have:
- Experienced a blood clot at a young age (i.e., before the age of 50) that was unprovoked.
- Strong family history of VTE, including a number of close relatives who had a blood clot under age 50.
- Recurrent blood clots, especially at a young age.
- Severe or extensive VTE or blood clots in unusual sites.
Some Testing Concerns
As with any medical decision, there are also concerns about testing, so screening for thrombophilia is an option that you and your healthcare provider should make together carefully. Should you decide to pursue testing, you should work together with your doctor and a genetic counselor. Together, they can help you understand your results and their implications.
Some considerations and cautions about testing include:
- Testing can be inaccurate. False positives and negatives are possible with these tests, although uncommon when the testing is conducted at the right time. To minimize inaccuracies, your physician will avoid testing you if you have an active blood clot or are taking blood thinning medications, are pregnant or taking estrogen hormonal therapy as these conditions are known to influence test results. Likewise, certain illnesses, like kidney and liver disease, can also affect test results.
- Results typically don’t affect treatment decisions. If you are already being treated for a blood clot, neither a positive nor negative thrombophilia testing result will likely alter your treatment plan. However, in the case of HAD, a prevention strategy is available since AT levels can be increased by the addition of AT factor. In the case of a confirmed thrombophilia diagnosis, your physician will continue your treatment with medications known as blood thinners. (See Section 7 for information about these medicines.) Of course, a negative thrombophilia test would be a relief. However, it’s critical that you don’t assume a false sense of security from the good news. You are still at risk based on your blood clot history. So, continue to take prescribed medication and follow all other medical instructions such a weight reduction as obesity is an important modifiable risk factor. If you are diagnosed with a thrombophilia and haven’t had a blood clot, it is unlikely that you will be given preventive treatment unless you have other significant risk factors. While all thrombophilias increase the risk for blood clots, overall risk remains low. For example, the general odds of experiencing a blood clot are approximately 1 to 2 per 1,000 people. If your thrombophilia increases this chance 5-fold, your risk is still only 1 percent or less. So, your doctor may not want to expose you to the potential side effects of blood thinners — including life-threatening bleeding — if your chance of a clot is low.
- Negative test results don’t mean you aren’t at risk. Sometimes people with extensive family histories test negative for thrombophilia. However, they remain at heightened risk for blood clots because VTE in close family members is a risk factor for a future blood clot. Yet, patients and/or their physicians may wrongly assume that negative test results minimize risk and may forego prudent preventive actions.
- Diagnosis can cause significant anxiety. If patients receive a diagnosis of thrombophilia in absence of other risk factors, it may cause them unnecessary anxiety even though the results may not change their overall risk profile. Unfortunately, many patients may worry excessively, lose sleep and have difficulty concentrating on work or family. In worst-case scenarios, some people pursue unnecessary treatment that exposes them to alternate risks. In most instances, a positive diagnosis is considered secondary to family history or personal experience with VTE. For most patients who have never had a blood clot, thrombophilia status is only considered relevant to prevention strategies when they face particular health events, such as surgery or pregnancy, that are established risk co-factors.
- Testing can be expensive. Some insurance plans won’t cover testing except under clearly defined circumstances that demonstrate medical necessity. Insurers are more likely to pay for tests if you have an abnormal blood clotting history, but not all do. Without coverage, testing – especially genetic screening – can be quite costly. Anyone considering thrombophilia screening should contact their insurance company to understand the criteria for coverage. Likewise, patients should know in advance their own financial obligations including co-pays, deductibles and out-of-pocket percentages. Although your doctor’s office and laboratory may handle much of the paperwork, make sure you are knowledgeable about the requirements.
Genetic Counseling
It is also important to seek the guidance of a genetics counselor when testing for thrombophilia. Genetic counseling services, or genetic counselors, can help families at risk for inherited conditions investigate the problem present in the family, interpret information about the disorder, analyze inheritance patterns, interpret risks to family members, review available management options, and help with insurance issues. For more information about genetic counseling, visit the following link: National Society of Genetic Counselors.
Testing Approaches
For many thrombophilias, the first tests performed are assays to measure the amounts and activity levels of the various clotting proteins. For proteins that play an active role in clot formation, unusually high levels would suggest that the body is producing either too much or an abnormal version of the molecule. For proteins that inhibit the clotting process or dissolve clots once blood vessel repair is complete, inadequate levels would show that the body is having trouble generating adequate amounts or properly functioning forms of the molecule. These types of assays are available specifically for antithrombin and proteins C and S. If results strengthen suspicion of an underlying thrombophilia, screenings for genetic mutations may be warranted.
For the most common thrombophilias, factor V Leiden and prothrombin G20210A, only genetic tests are available to identify the presence of characteristic mutations. The most common tests use technologies that multiply the DNA in a blood sample into millions of copies so that mutations can be easily identified.
Antiphospholipid antibodies are strictly an acquired thrombophilia, so no genetic screenings are necessary. Instead, several assays are used to detect antibodies, such as anticardiolipin and B2-glycoprotein along with assays to detect the functional presence of other antibodies associated with antiphospholipid disorders.
Privacy and Discrimination
It would be normal to worry about the impact of genetic testing – particularly a confirmed thrombophilia diagnosis – on your ability to secure health and other insurance. Thanks to aggressive legislative efforts by the Federal government and many states, you are protected from discrimination by employers, insurance companies and others based on your genetic information. Likewise, the sharing of this information is strictly regulated. For more on this subject, click this link from the National Human Genome Research Institute (NHGRI): https://www.genome.gov/10002077/

Treatment & Prevention
Blood Clot Treatment and Prevention
Blood clots are managed with anticoagulants, also known as blood thinners. Although these medications don’t actually dissolve the clot, they do slow down the clotting process by binding to various clotting proteins and neutralizing them or reducing the production of clotting proteins by the liver.29 This keeps existing clots from getting larger and stops the formation of new clots while the body works to dissolve the existing clot. In certain severe cases, very strong blood thinners that will dissolve a clot more quickly than the body may be considered. If you experience a blood clot, you and your doctor will work together to select a suitable blood thinner and develop a treatment plan based on the location, extent and severity of the clot, your risk for bleeding and other considerations of your overall risk profile.30 The goal will be to maximize treatment benefits while minimizing adverse effects. It is important that you take medication as directed, comply with all monitoring requirements, and report any potential complications immediately to your health professional.

Sometimes blood thinners are prescribed strictly for primary clot prevention in people who have multiple risk factors, including a known thrombophilia, a strong family history of VTE, and a current health issue – such as pregnancy, hospitalization or impending surgery or prolonged immobilization – that are correlated with a higher incidence of clotting. Individuals with HAD may also receive additional antithrombin in high risk situations.
Blood thinners are highly effective but may cause side effects, including moderate to severe bleeding and heavier menstrual cycles. Some of these therapies require periodic monitoring to ensure that they’re working consistently.
The following are summaries of the most commonly prescribed blood thinners:
Unfractionated Heparin (UFH)
Unfractionated heparin (UFH) is a fast-acting anticoagulant that suppresses blood clot formation soon after administration.
Due to its rapid onset of action, UFH is normally the emergency treatment of choice for blood clots that are diagnosed in a hospital setting. It is typically given intravenously (IV), so it is not given in the outpatient setting. Shots of unfractionated heparin are prescribed for patient self-administration, but only in rare circumstances.
UFH therapy given through an IV requires strict and frequent monitoring to ensure adequate blood levels. Initial dosing is based on the patient’s weight. UHF needs antithrombin to be effective, so people who have HAD may need to be treated with additional antithrombin in order to achieve therapeutic levels with UHF therapy.
Heparins don’t cross the placenta, so they are considered safe to use in pregnant women, although low-molecular weight heparin (see below) is considered the optimal formulation for various reasons.
Before starting UFH treatment, you should alert your physician if you are taking a pain medication, such as aspirin, ibuprofen, naproxen or any other non-steroidal anti-inflammatory drug (NSAID) as these increase bleeding risks.
Low-Molecular Weight Heparin (LMWH)
An alternative formulation of heparin, low-molecular weight heparin (LMWH) offers advantages similar to UFH, but with a few significant differences. LMWH is fractionated, a process that separates and collects the smallest molecular chains of heparin. These tiny strands act more predictably and last longer than UFH molecules. As a result, LMWH doesn’t require the frequent blood tests necessary with UFH. LMWH is usually administered via skin injection, making it more suitable than UFH for home use.
Given its longer activity, however, LMWH can be more difficult than UFH to reverse should bleeding occur. Also, some patients may find home injections difficult to self-administer. From a cost perspective, LMWH is more expensive than UFH and may be an additional burden to patients without adequate insurance coverage.
For pregnant women requiring heparin therapy, LMWH is the preferred heparin formulation.
LMWH is often used as a bridge therapy between UFH and an oral anticoagulant, such as warfarin (see below).
LMWH needs antithrombin to be effective, so people who have HAD may need to be treated with additional antithrombin in order to be successful with LMWH therapy.
Before starting LMWH treatment, you should alert your physician if you are taking a pain medication, such as aspirin, ibuprofen, naproxen or any other non-steroidal anti-inflammatory drug (NSAID) as these increase bleeding risks.
Warfarin
People who require intermediate to long-term therapy with blood thinners are often prescribed warfarin (Coumadin), an anticoagulant used successfully since the 1950s.
Warfarin is taken orally, so it is highly suitable for home use and eliminates the need for painful and inconvenient injections or infusions. Its once-daily formulation improves patient compliance, a critical concern for outpatient blood clot management. Although warfarin can cause bleeding characteristic of all blood thinning drugs, its effects are easily reversed in the event of complications.
Warfarin dosing is individualized and not based on weight. Therefore, it requires frequent monitoring by a test called the prothrombin time or PT. The PT measures the time it takes for blood to clot. The PT test is used to make sure the patient is taking the right dose of warfarin. The PT is reported by labs as an International Normalized Ratio or INR. For most patients, the ideal INR range is between 2.0 and 3.0. Readings lower than 2.0 increase the chances for clot formation and results above 3.0 elevate the risk for bleeding.
Warfarin crosses the placenta and thins the blood of the fetus and therefore should not be taken by pregnant women except in very limited circumstances. Warfarin is the best blood thinner for patients with mechanical heart valves so women with heart valves should discuss their management with their cardiologist and obstetrician before becoming pregnant. Warfarin is not found normally in breast milk, so it is suitable for nursing moms.
Many foods interact with warfarin, especially foods high in vitamin K, such as many green leafy vegetables. Alcohol can also affect warfarin levels, so patients who drink should consume no more than 1-2 daily servings.
As with all anticoagulant therapy, NSAIDs such as aspirin and ibuprofen should be avoided when taking warfarin. Notify your doctor if you currently use any of these medications before beginning a warfarin regimen.
Direct-Acting Oral Anticoagulants (DOACs)
Direct-acting oral anticoagulants (DOACs), offer a mix of short- and long-acting agents with good safety profiles and relatively low bleeding risks. The medications have been extensively studied and are considered to be at least as effective as conventional treatments.31 Members of this class of compounds include apixaban (Eliquis), betrixaban (BevyxXa), dabigatran (Pradaxa), edoxaban (Savaysa) and rivaroxaban (Xarelto).
DOACs block various proteins that are instrumental to the production of fibrin, an essential component of blood clots. They perform predictably at fixed doses so they do not require routine monitoring.32 DOACs also have fewer medication and food interactions than standard therapies.
There is limited information on DOACs during pregnancy but animal studies suggest they may cause adverse effects, so they should be avoided in pregnant women.34 Likewise, they should be used with caution in people with kidney or liver impairment. In the setting of antiphospholipid syndrome (APS), DOACs are generally not preferred, and the choice of blood thinner needs to be discussed in detail with a specialist familiar with APS. Dabigatran and the anti Xa inhibitors do have antidotes available, but not all hospital systems carry all products. As a result, the ease of reversibility of blood thinners is part of the decision-making with your health care provider when choosing a medication right for you.
Again, anyone prescribed DOACs should notify their physician if they are taking aspirin or other NSAIDs for pain relief as they increase bleeding risks.
Reducing Risk
Lifestyle Changes to Reduce the Risk for Blood Clots
For people who have experienced a blood clot or have been told by a healthcare professional that they are at elevated risk for DVT or PE, various lifestyle adjustments can provide added protection. Overall, it is important to stay healthy and active. Drink plenty of fluids, preferably water, to avoid dehydration. Eat a balanced diet, incorporating a variety of nutritious foods that do not interfere with the effectiveness of any blood thinners you might be taking. Choose exercises, sports and other activities that you enjoy and that are appropriate for your health status. Exercise keeps your blood moving and maintains good circulation. It also helps you to lose or maintain body weight and improves lung function.
Periods of extended immobility, such as very long plane flights or extended intervals of sedentary behavior (e.g., sitting at your work desk or on the couch watching TV) are known to heighten the chances for a blood clot. When travelling, especially on overseas trips, try not to stay confined in your seat for the duration. When the “no seat belt” sign is lit, go into the aisle periodically to walk or stretch. If you must stay seated, avoid crossing your legs because this weakens circulation. Likewise, you can do foot and ankle exercises with minimal movement, such as rotating your ankles or pumping your feet. The latter involves putting your feet flat on the floor and alternately raising your toes and heels.
These exercises can also be useful if you’re stuck at your work desk many hours each day. Likewise, it’s a good idea to set your cell phone alarm as a reminder to stand and walk down the hall every hour or two. If your schedule allows, go outside for lunchtime instead of ordering in food.
If you’re a person with a demanding desk job or extensive travel requirements, talk to your physician about compression stockings that are designed to put gentle pressure on your legs and feet to improve blood flow.

Quitting smoking is one of the best changes you can make for overall health and, particularly, for reducing blood clot risks. Smoking constricts blood vessels and, in combination with a fatty diet, increases plaque development on vessel walls. All of these physical effects make a blood clot more likely. If you are using blood thinners, make changes that reduce the likelihood of cuts and other injuries that could bleed excessively. First, avoid activities that increase these dangers, such as contact sports. If you ride a bicycle, ski or skate, make sure you wear customary safety equipment to protect from injury.
In the home, switch to electric razors when shaving. Be extra careful when cutting nails and hair with clippers or scissors. Learn and practice safer methods for chopping and slicing food while cooking. Consider kitchen tools designed to reduce the need for cutlery, such as food processors and hand-held dicers with shielded blades. For oral care, use a soft- or extra-soft toothbrush and waxed floss to minimize gum bleeding. Talk to your healthcare provider about other sensible steps you can take to lower blood clot risks.

VIEW A NEW VIDEO ABOUT FAMILY HEALTH HISTORY AND GENETIC CLOTTING BELOW:
VIEW THE VIDEO ABOUT THROMBOPHILIA & PREGNANCY BELOW:
VIEW THE VIDEO BELOW FOR AN OVERVIEW ABOUT THROMBOPHILIA:
On May 11, 2021, NBCA hosted a Facebook Live Event about thrombophilia and pregnancy. Below you can tune into the discussion between Dr. Rachel Rosovsky, a former member of NBCA’s Medical and Scientific Advisory Board, and her patient, Kate Leflar, about this important topic.
On August 26, 2021, NBCA hosted a Facebook Live Event about thrombophilia and pregnancy. Below you can tune into the discussion between Dr. Rachel Rosovsky, former member of NBCA’s Medical and Scientific Advisory Board, and a patient panel about this important topic.
Discuss any questions you might have with your healthcare team, and get additional information from a genetic counselor. Click here to identify a genetic counselor in your local community.

Development made possible with funding from Grifols USA, LLC
