I have never been “normal” when it comes to my health as a young adult. For 10 years, I struggled with severe stomach and esophagus problems. I developed an allergy to the medication that treats the conditions in my esophagus. So, this year, my health finally ran out of options. It wasn’t until April 2018 that I found a team of specialists to take on my case to work towards establishing a better quality of life. In July 2018, I found a cardio thoracic surgeon to perform a laparoscopic Nissen fundoplication and hiatal hernia repair. The recovery was tough, as I learned how to swallow and was only able consume clear liquids. I also wasn’t allowed to lift my one-year old son to avoid undoing the procedure, so I was limited with my mobility.
One week after being discharged from the hospital, I was taking one of my evening walks. As cautioned by my surgeon, I was adamant about never letting myself be less active than the day before. I got down the stairs of my apartment and felt as though I pulled a glute muscle. I figured I overdid it for the day and went to bed. The following morning, I was still struggling with what felt like a pulled muscle. As the day progressed it became harder to walk. I took it easy that evening on the couch, hoping that would give my body a break. At 7:00 p.m. I could not get off the couch, and by 9:00 p.m. my leg had doubled in size right before my eyes.
I was admitted to the hospital that night with an obvious deep vein thrombosis or DVT in my left leg. My toes to my groin were terribly red and swollen with pain, numbness, and tingling. Everyone figured I would be on a heparin drip for a few days and then be back to normal. I just had a major surgery with an inactive recovery, so it wasn’t outrageous that I developed a blood clot.
The following night chest pains started, and I couldn’t breathe. Multiple times throughout the night I required assistance from the rapid response team to help me restore my breathing. The next morning, they did tests to confirm that I had bi-lateral pulmonary embolisms, or blood clots in my lungs, as well as another DVT in my left arm. I was officially transferred to the ICU, which would be my new home over the next few weeks.
I had a vascular surgeon perform my first surgery to remove the clot. That didn’t work. My leg was still visibly growing in size. During a second surgical procedure I had a catheter, stent, and IVC filter placed, since my condition was worsening. Since I was only 25 years old, my surgeon wanted to treat it aggressively to give me a better hope of recovery. It still did not work. The night before a third surgery, my platelet counts dropped significantly. My leg was still clotting. During that surgery it was discovered that not only was I experiencing type 2 heparin induced thrombocytopenia, or type 2 HIT, which is an allergy to heparin, but I also had severe May-Thurner Syndrome. This explained the feeling of a pulled muscle I exhibited in the beginning. The surgeon corrected it and placed a stent in my vein.
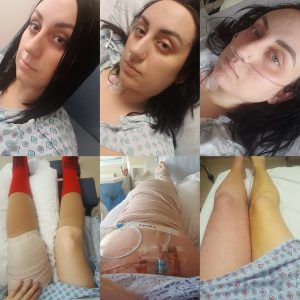
My leg was still clotting. The clotting had gone all the way up into my abdomen. We officially requested a transfer to a larger hospital that had more access to specialized vascular equipment. The team got the type 2 HIT under control with argatroban. The next morning, they performed an intense clot evacuation. I still remained a patient in the ICU. The following days were quite a blur as I was experiencing ICU delirium. I required two blood transfusions and was on a PCA pump. Once I finally started to show signs of improvement, I was moved to a regular hospital room.
I spent a total of 25 days in the hospital during the month of August. I had to learn how to walk again. I was discharged with home health care since I am not strong enough to care for myself after the damage my body sustained. I get around with compression socks and a cane, and I require use of a wheelchair for doctors visits or grocery shopping, since my lungs are still in the early stages of recovery. I’m receiving physical and occupational therapy on a regular basis to help me learn how to function after DVT, PE, and May-Thurner Syndrome.
I’m slowly learning there are positives after these life-altering events. I’m constantly being reminded that I’m lucky to be alive. According to my hospitalist, I had “youth on my side” because if I was any older, the outcome would not have been favorable due to the severity of my situation. I have a long road ahead of me full of weekly blood tests, and many medications to take, such as blood thinners and antiplatelets to prevent any future episodes. I’m taking life one day at a time and learning to appreciate the amount of stress the human body can sustain and overcome despite the odds.
Every day is a struggle, but every day does get easier. I wish I had been more educated about blood clots. I feel as though I wrote them off as an “old person” condition, which is most certainly not the case. I had the perfect storm of factors that caused this situation to happen at my young age, but it was actually a blessing in disguise. May-Thurner Syndrome is a rare vascular condition that is not usually diagnosed without visually looking at the compressed vein. If it wasn’t for my initial surgery to correct my digestive issues in July, this could have gone undiagnosed for years, and maybe my heart would not have been as youthful to save me by that time.
My messages for people who read my story:
- Educate yourself. Don’t ever assume you are untouchable from these conditions.
- Advocate for yourself. If you know something is wrong with your body, do not stop until you are heard and get answers. Question your doctors. They may have the medical degree, but you know your body best.
- DVTs can present as a pulled muscle. Do not wait to seek medical attention. This is treatable if appropriate and timely measures are taken.
- May-Thurner Syndrome is not typically diagnosed until after a blood clot occurs.
- DVTs, PEs, and May-Thurner Syndrome are life-altering and sometimes deadly conditions, but there is life after blood clots.
MORE INFORMATION AND RESOURCES:
- Join our online peer support community to connect with other people who have experienced a blood clot.
- Read more about May-Thurner Syndrome.
- Read more stories, or share your story with NBCA.




