Low Molecular Weight Heparin (LMWH)
 Low molecular weight heparin (LMWH) is derived from unfractionated heparin (UFH) by digestion or depolymerization of longer chains of heparin into shorter chains by chemical or enzymatic means. These short strands make LMWH last longer and act more predictably in the body than UFH.
Low molecular weight heparin (LMWH) is derived from unfractionated heparin (UFH) by digestion or depolymerization of longer chains of heparin into shorter chains by chemical or enzymatic means. These short strands make LMWH last longer and act more predictably in the body than UFH.
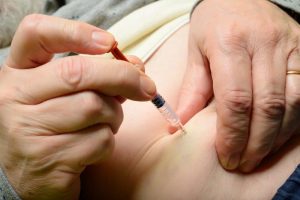
Although LMWH and UFH work similarly to inhibit clotting factors, LMWH can be self-administered at home via subcutaneous (under the skin) injection and does not require regular blood monitoring necessary for UFH treatment. As with all heparins, LMWH dosing is based on a patient’s weight. LMWH options available in the United States are dalteparin (Fragmin) and enoxaparin (Lovenox).
Advantages of LMWH
- Longer and more predicable activity than UFH
- Self-administered at home via subcutaneous injection, reducing or eliminating hospital stays
- No regular blood monitoring required
Disadvantages of LMWH
- Expensive
- Can be uncomfortable to administer, especially if a patient is fearful of needles
- Longer activity can complicate reversal, if necessary
Potential Side Effects of LMWH
- Uncontrolled bleeding (most serious side effect)
- Injection site reactions such as redness, irritation and bruising
- Loss of bone strength (less than UFH)
- Elevated liver enzymes
- Heparin induced thrombocytopenia (HIT)
Long-term use of UFH is associated with a 2% incidence of bone fracture after nine months of administration. It remains unclear whether LMWH is also associated with osteoporosis. However, LMWH should be used cautiously for long-term treatment until this risk is further clarified. Heparin-induced thrombocytopenia (HIT) is also a risk, but it is much less common with LMWH than with UFH.
Heparins do not cross the placenta or harm the fetus, so they are the preferred anticoagulants for pregnant women who experience – or who are at heightened risk of – blood clots. LMWH is the heparin of choice in obstetrics due to its lower incidence of bleeding and other complications in pregnancy when compared to UFH. Likewise, LMWH is also the favored treatment for cancer-related blood clots, since it has been shown to be more effective than warfarin.
LMWH is often used temporarily to help patients transition – or bridge – to long-term oral anticoagulant therapy, most commonly warfarin or Coumadin. Your doctor will usually add warfarin to your medication schedule, so you take both warfarin and LMWH for several days under careful monitoring. Once your body achieves therapeutic blood levels of warfarin, your doctor will discontinue LMWH injections.
As with UFH, let your doctor know if you are taking aspirin, other non-steroidal anti-inflammatory drugs (NSAIDs) – such as ibuprofen or naproxen – or clopidogrel before starting LMWH treatment, because these drugs increase the risk of bleeding.
There are no known food interactions or dietary restrictions with LMWH. Calcium and vitamin D supplementation are often prescribed to help prevent bone loss. If you are taking LMWH long term, it is a good idea to wear or carry identification stating you are taking LMWH in case of a medical emergency.
What’s Next:
- Read more about warfarin
- Read more about pregnancy, childbirth, and the prevention of blood clots
- Return to NBCA’s Blood Clot Treatment Page for more information




